- It’s a non-invasive treatment administered by trained chiropractors, osteopaths and other certified healthcare professionals. This type of therapy doesn’t involve any invasive surgery or pharmaceutical medications.
- Spinal decompression therapy involves the practitioner deliberately stretching the spine and restoring its natural health using specialized equipment. The ultimate goal is to help relieve back, neck and leg pain over time. Spinal decompression therapy is a long-term approach to treating patients naturally in an environment that supports the individual’s health and wellness goals.
If you are considering spinal decompression therapy for your neck or back conditions, you should know what to expect during your treatments:
- You remain fully clothed during your treatments.
- Treatment times vary between 15 minutes to 30 minutes, however, some cases may require other therapies, such as chiropractic treatments, exercise, and muscle stimulation that would add time to your office visit.
- During treatment, you may be positioned on your back or face down, depending on your condition.
- Treatment is slow and controlled. Most patients find the gentle pulling of the decompression table very relaxing.
Spinal decompression treats conditions involving the disc and spinal cord. Some patients may only experience one symptom, while others may develop more over time as their chronic condition persists untreated. These conditions cause many different types of symptoms which include:
- “Pinched” nerves
- Neck pain
- Pain at the base of the skull
- Upper back and shoulder pain
- Arm pain
- Lower back pain
- Pain radiating down the legs
- Pain in the hip or buttock
- Muscle spasms
- Numbness and tingling
- Burning pain
- Decreased mobility in the spine
Because every case is different, we tailor our treatment plans to the needs of each individual patient. Generally, the total treatment ranges from 6 to 8 weeks and may require anywhere from 15 to 35 visits. We initially recommend 4 or 5 treatments per week for the first 2 or 3 weeks to see any improvement, then tapering off as your spine begins to stabilize.
Traditional decompression tables pull in one direction. While many patients respond quite well to this, some require more specific targeting to address their problem. With 3D decompression, the table allows the practitioner to also comfortably laterally bend, rotate, flex, and extend their patient’s spine during treatment. This allows them to target not only the affected disc(s), but targeting a specific area of the disc. This allows the practitioner to use less force and less treatments to achieve results.
Currently, there are only a handful of 3D spinal decompression systems available. After months of research, Carver Chiropractic decided on the DOC 3D decompression system. This table allows us to treat the widest variety of cases and allows us to reproduce each treatment with complete accuracy using the computerized programming system.
Decompression therapy is common among chiropractors, osteopaths, physical therapists, and pain management clinics. The treatments are typically administered by the doctor, nurse, or physician/chiropractic assistant.
It is important to ask your practitioner about their training on the decompression system. Obviously, the more training your practitioner pursues, the better outcomes he/she will get. Our office has completed a full training course on 3D decompression.
- As the Spinal Decompression table pulls, it gently separates the vertebrae from each other, creating a vacuum inside the discs that we are targeting. This vacuum begins to suck the bulges or herniations back into the inside of the disc, and off of your nerve root. It happens only microscopically each time, but cumulatively the results are quite dramatic.
- Also, this pumping action pumps nutrient-rich fluids from the outside of the discs to the inside. These nutrients enable the
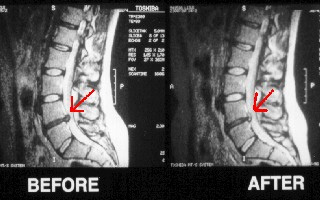 torn and degenerated disc fibers to begin to heal back up.
torn and degenerated disc fibers to begin to heal back up. - Only a few years ago, it
was thought that once a disc was degenerated, there was nothing you could do. Now we routinely see discs gain one to two millimeters of sustained increased disc height. While this may not seem like much, it can make all the difference in the world for your nerves.
Yes. Our table is one of the few available that uses “active decompression.” This means that the table and the patient move together to achieve decompression.
This is not like the older “pulley system” units of the past where belting systems are attached to a winch-like motor, similar to a fishing reel.
This system allows the actuator-controlled table to measure the body’s resistance and adjust accordingly. This greatly reduces the occurrence of muscle spasms.
Spinal decompression therapy is an effective treatment for anyone who suffers from disc-related pain that causes symptoms in the neck, back, or extremities.
If you’ve been told you need surgery and wish to avoid it, if you’ve tried other options like injections, physical therapy, and even surgery and are still in pain, you may be a candidate for spinal decompression.
We recommend this treatment for 3 categories of injury:
- Acute Disc Pain – Newly injured discs tend to respond very well to decompression. These injuries may include auto accidents, sporting accidents, slips, falls, etc. The faster the injury is treated, the more likely it is to recover quickly and completely.
- Chronic Disc Pain – Patients with chronic disc conditions have most likely been dealing with symptoms and pain for several months or years. Some common causes of chronic disc conditions are arthritis, degeneration, repetitive injuries, and over-use. These patients’ treatment plans are typically longer than acute injuries due to the long-standing damage to the discs.
- Acute Flare-Up of Chronic Pain – These patients have dealt with disc injury in the past, and may not be experiencing symptoms. Usually, it is a simple movement that causes the flare-up. Bending over to tie shoes, getting out of bed, stepping up/down stairs. These simple tasks can usually cause lots of pain during a flare up because the disc has never fully healed and is prone to re-injury.
No. There are certain conditions which would prohibit you from using spinal decompression. The most important part of your therapy is a thorough examination. During this examination, your doctor will determine if you would respond to decompression therapy, and develop a unique treatment plan according to your condition. Some conditions that may not be appropriate for decompression therapy include fractures, tumors, metal implants, severe osteoporosis, and pregnancy.
If you’ve had X-Ray or MRI studies performed, bring them with you to your consultation. If not, your doctor will most likely perform imaging during your examination.
No. We’ve found that the minimum time for treatments to be effective is 15 minutes. This is essentially impossible to accomplish on an inversion table. True decompression cycles through a series of pull/relax movements. This is how the discs are rehydrated and repaired. Also, for treatment to be effective, we use a specific amount of force depending on the treatment area. Also impossible with inversion. For these reasons, we do not recommend inversion therapy for any of our patients.
Yes! There have been many clinical trials over the years that prove the efficacy of spinal decompression. Here’s just a couple:
Serial MRI of 20 patients treated with the decompression table shows in our study up to 90% reduction of subligamentous nucleus herniation in 10 of 14. Some rehydration occurs detected by T2 and proton density signal increase. Torn annulus repair is seen in all.
Eyerman, Edward MD. Simple pelvic traction gives inconsistent relief to herniated lumbar disc sufferers. Journal of Neuroimaging. Paper presented to the American Society of Neuroimaging, Orlando, Florida 2-26-98.
82% of selected patients reported improvement after only two weeks of 3D decompression treatments with exercises than the exercise only group, Decompression group displayed greater improvements in disability (mean adjusted ODI difference of 7.2 points) and fear-avoidance (mean adjusted FABQ difference 2.6 points) at 2 weeks.
Fritz JM et al. Is there a subgroup of patients with low back pain likely to benefit from mechanical traction? Results of a randomized clinical trial and subgrouping analysis. Spine 2007; 32(26): E793-E800


